COVID-19 contact tracing emerging as controversial balm as search for cure continues
August 31 - September 6, 2020
By Daily Record Staff
As local schools return to class and more adults leave their remote working environments at home and head back to office, contact tracing is increasing part of the national conversation as communities frantically seek ways to combat and slow the spread of COVID-19.
Ever since the World Health Organization declared the SARS-CoV-2 virus a global pandemic, contact tracing has emerged as possible antidote to reduce COVID-19 infections and enhance the medical community’s response by quickly identifying, monitoring or quarantining persons who may have come into contact with someone infected with an illness.
Advocates of the practice, including the U.S. Centers for Disease and Control, say the deployment of various methodologies is crucial to slowing the spread of COVID-19 by informing and counseling individuals that they may have been exposed to the virus. For COVID-19, a close contact is defined as any individual who was within 6 feet of an infected person for at least 15 minutes starting from 48 hours before the person began feeling sick until the time the patient is isolated.
A recent report by New York City-based Human Technology Foundation (HTF) details some of those legal, healthcare and technology concerns about contact tracing. Doron Goldstein, a partner at Wall Street law firm Katten and a contributor to the foundation’s “Technology Governance in a Time of Crisis” report, noted that contact tracing not only raises privacy concerns but also a range of other legal and ethical challenges, including issues of accessibility, transparency and discrimination.
“COVID-19 has exposed both the challenges and benefits of technologies that can be used for contact tracing, and the report gives examples of how best to do that,” said Goldstein, co-head of Privacy, Data and Cybersecurity at the New York City law firm. “One of the things about the pace of technology and technological implementation is that you can’t sit back. It’s a constant process, and it is key to spend the time at the outset to think through both the positives and the challenges of using a new technology.”
The HTF report also identifies how contact tracing technology can be deployed in a manner that will help reassure users rather than leave them suspicious and worried about the use of their personal information. One key element of the report is that it gives examples and tools for decision-makers — both in the private and public sectors — to try to balance the concerns of individuals and public health and safety needs.
“Privacy and data concerns have been widespread for quite a while, but the concerns are even more heightened during these uncertain times,” said Goldstein, who was part of a team of technologists, attorneys and ethicists from 13 countries that contributed to the report. “One of the key individual concerns about contact tracing processes is that — by their very nature — they need to have some form of location-based tagging, so it means that someone or something knows where you have been, and those with whom you’ve interacted.
Here in central Arkansas and across the state, experts in education, healthcare and the technology sectors are also asking the same questions and raising similar concerns as their professional peers across the U.S. and globally. On Aug. 18, the New York Institute of Technology College of Osteopathic Medicine (NYITCOM) reached an agreement with the Arkansas State University System to conduct COVID-19 contact tracing for each of the system’s campus locations across the state.
The osteopathic medical school, which is house on A-State’s main campus in Jonesboro, will use its own medical staff, community partners and the Delta Population Health Institute (DPHI) to execute the initiative. The A-State fall semester began Aug. 24, and the contact tracing infrastructure will be in place when students return to campus.
“We’re very fortunate to have an outstanding medical school located in the heart of our campus in Jonesboro,” said ASU System President Chuck Welch. “Dean Speights and the NYITCOM team are providing a critical service to our ASU System institutions and communities with COVID-19 tracing work. Their guidance to us during this pandemic has been extremely helpful, and we’re grateful for this partnership.”
Dr. Speights, NYITCO’s dean, said his staff is now working closely and coordinating with the state Department of Health to follow all proper protocols and procedures as students begin returning to ASU’s main campus in Jonesboro, as well as five independently accredited and functionally separate two-year institutions headquarter in Beebe, Malvern, Mountain Home, Newport and West Memphis.
The A-State system also includes a satellite campus in Queretaro, Mexico. Further, the board of trustees for Arkansas’ second-largest university approved a merger agreement and transition plan in late 2019 with the financially strapped Henderson State University in Arkadelphia, which is now the system’s seventh higher education affiliate.
Under the new COVID-19 contact tracing pact, students, faculty and staff in the ASU System will be required to report if they are positive, exposed or symptomatic. NYITCOM’s contact tracers will then connect with those who have been exposed to a positive case as well as unconfirmed symptomatic persons to provide guidance for care. Dr. Brookshield Laurent, who chairs NYITCOM’s department of clinical medicine will lead the project. She also serves as executive director of DPHI, the medical school’s initiative on the ASU campus to improve health outcomes in the Delta.
“This is about providing a safe learning and working environment for students, faculty and staff,” Laurent said. “As students return to campus, it’s inevitable that there will be cases of COVID-19. By effectively and efficiently implementing the proper protocols, we will diligently work to limit the spread and keep everyone as safe and healthy as possible.”
Speights told the Daily Record that NYITCOM and ASU officials began discussing ways to provide COVID-19 support to the main campus in Jonesboro in the spring. Those talks expanded six to eight weeks ago to develop a COVID-19 mitigation plan for students across the entire ASU system to return safety to all eight campuses, which includes more than 40,000 students, faculty, administrators, staff and other personnel.
“We wanted to make sure we had the bandwidth and we had the resources to do this, so we had to look internally and make sure we do it even though there may not be funding for something like this,” said Speights. “But we felt it was the right thing to do for our partner and out community, so we agreed to support them on that.”
The NYITCOM dean said the medical school’s contact tracing model for the ASU system is taken from COVID-19 best practices from across the globe. Beside medical school faculty and staff to help with the project, the osteopathic college also operates ASU’s on-campus medical clinic and will train that staff on COVID-19 testing and tracing protocols.
NYITCOM will also hire about 60 temporary workers to serve as contact tracers and case investigators for the partnership, which will be fully funded by the medical school. The state Health Department will partly fund the testing piece of the project, he said.
National testing, tracing plan still on the shelf
Even with careful planning, critics and advocates of COVID-19 contact tracing offer a wide range views on the expansion of statewide or national strategy like the ASU model. For example, the Rockefeller Foundation pitched a national COVID-19 testing plan in April that could remain in place as long as it takes to develop a vaccine or cure.
“Testing is our way out of this crisis. Instead of ricocheting between an unsustainable shutdown and a dangerous, uncertain return to normalcy, the United States must mount a sustainable strategy with better tests and contact tracing, and stay the course for as long as it takes to develop a vaccine or cure,” said Rajiv Shah, president of the New York City-based private foundation established by the sixth-generation Rockefeller family. “Any plan to do so must win the faith of private and public sector leaders across the country, and of individual Americans that they and their loved ones will be safer when we begin to return to daily life.”
The foundation’s National Covid-19 Testing Action Plan lays out the precise steps necessary to enact robust testing, tracing, and coordination to more safely reopen the U.S economy – starting with a dramatic expansion of testing from 1 million tests per week to initially three million per week and then 30 million per week. That rollout would be backed by a national network to coordinate and underwrite the testing market, a public-private testing technology accelerator, and a national initiative to rapidly expand the use of university, government and local medical laboratory capacity.
“Together, we can do this. This action plan benefits from and builds on prior proposals, current efforts, and the broad participation of experts from so many fields,” said Shah, whose national plan has gained no suitors. “Enacting it will require strong leadership and collaboration: across states, cities, and federal government, and from businesses, nonprofits, universities, community groups, and individuals.”
Others are not so sure, especially concerning the contact tracing mobile technology and applications. In a late May, the progressive Brookings Institute in Washington, D.C., released a study highlighting most Americans are deeply skeptical of such technology.
Results of that nationally study of 2,000 Americans found that only 30% of Americans indicated they would download and use a mobile contact-tracing app, raising questions about whether such technology will be adopted widely enough to be effective. The survey also noted that support for digital contact tracing tends to increase with stronger privacy protections.
“Our survey indicates significant levels of distrust toward the technology companies and public health authorities administering contact-tracing technology, but when we described the way that some companies are trying to build contact-tracing tools with privacy and security in mind, we find significantly higher levels of support for apps,” stated Sarah Kreps, a professor of government and Milstein Faculty Fellow in Technology and Humanity at Cornell University.
For such tools to be effective, some 60% of the U.S. population would need to opt-in and use a mobile app or similar technology, the Brookings study notes. In April, the U.S. Census estimated that the U.S. population reached 8328.2 million on July 1, 2019, meaning for contact tracing to be effective about 196 million Americans would have to agree to be tracked and traced by a mobile app or other similar technology.
In late July, the Trump administration announced plans to accelerate efforts to find a COVID-19 cure when the number of positive cases first topped 1,000 deaths a day and 4.5 million cases. As a part of the administration’s “Operation Warp Speed” initiative, the National Institutes of Health (NIH), began two Phase 3 clinical trial designed to evaluate if an investigational vaccine can prevent symptomatic coronavirus in adults.
The first vaccine, known as mRNA-1273, was co-developed by the Cambridge, Massachusetts-based biotechnology company Moderna Inc., and the NIH. That trial is being conducted at 89 U.S. clinical research sites and has a goal of enrolling nearly 30,000 adult volunteers who do not have COVID-19.
Also, pharmaceutical giant Pfizer Inc. and smaller partner BioNTech SE have also started a global Phase 2/3 safety and efficacy clinical study to evaluate a single drug candidate from their vaccine program against SARS-CoV-2. In early March, Foster City, Calif.-based Gilead first announced that the U.S. FDA had fast tracked remdesivir for the treatment of COVID-19 and initiated two Phase 3 clinical studies to evaluate the safety and efficacy of drug in adults diagnosed with the novel coronavirus.
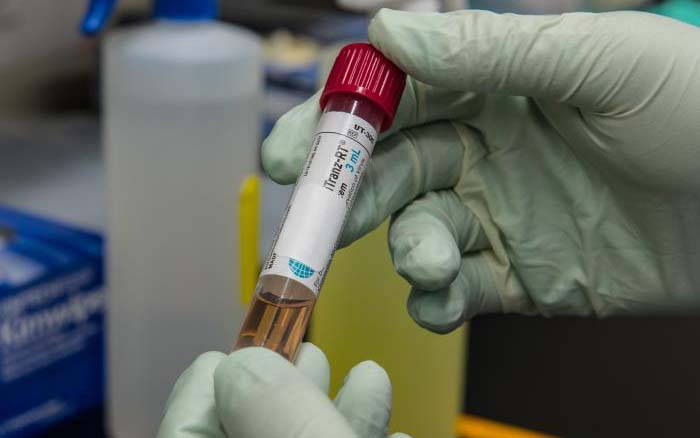
PHOTO CAPTIONS: (Photos provided by U.S. Centers for Disease and Control)
1. CDC and other advocates say contact tracing is key to slowing the spread of COVID-19 until cure or vaccine is found.
2. A CDC worker holds a test tube with viral transport media that contained a patient’s sample to be tested for the presence of SARS-CoV-2, the virus that causes COVID-19.